In vitro fertilization (IVF)
What is IVF
In vitro fertilization (IVF) means that the fertilization between the oocyte and the sperm takes place in a laboratory environment (in vitro). Vitro comes from the latin word vitrum (glass). IVF is an assisted reproduction technique (ART) together with several other procedures where laboratory/clinical procedures aid in reproduction. In Europe more than 1 million cycles are performed each year. Around 4 % of all babies born in Sweden are IVF babies and more than 20,000 IVF cycles are performed annually.
History
The pioneers in IVF are the biologist/physiologist Robert Edwards and the clinician Patrick C. Steptoe. Robert Edwards started research on human IVF already in 1963 and in 1978, after many human attempts, Edwards and Steptoe could eventually announce the first live birth after IVF, when Louise Brown was born in England. Robert Edwards was awarded the Noble prize in Physiology or Medicine in 2010 for the scientific achievement to develop IVF. The first IVF baby in Sweden was born in 1982.
Gonadotropin stimulation in IVF
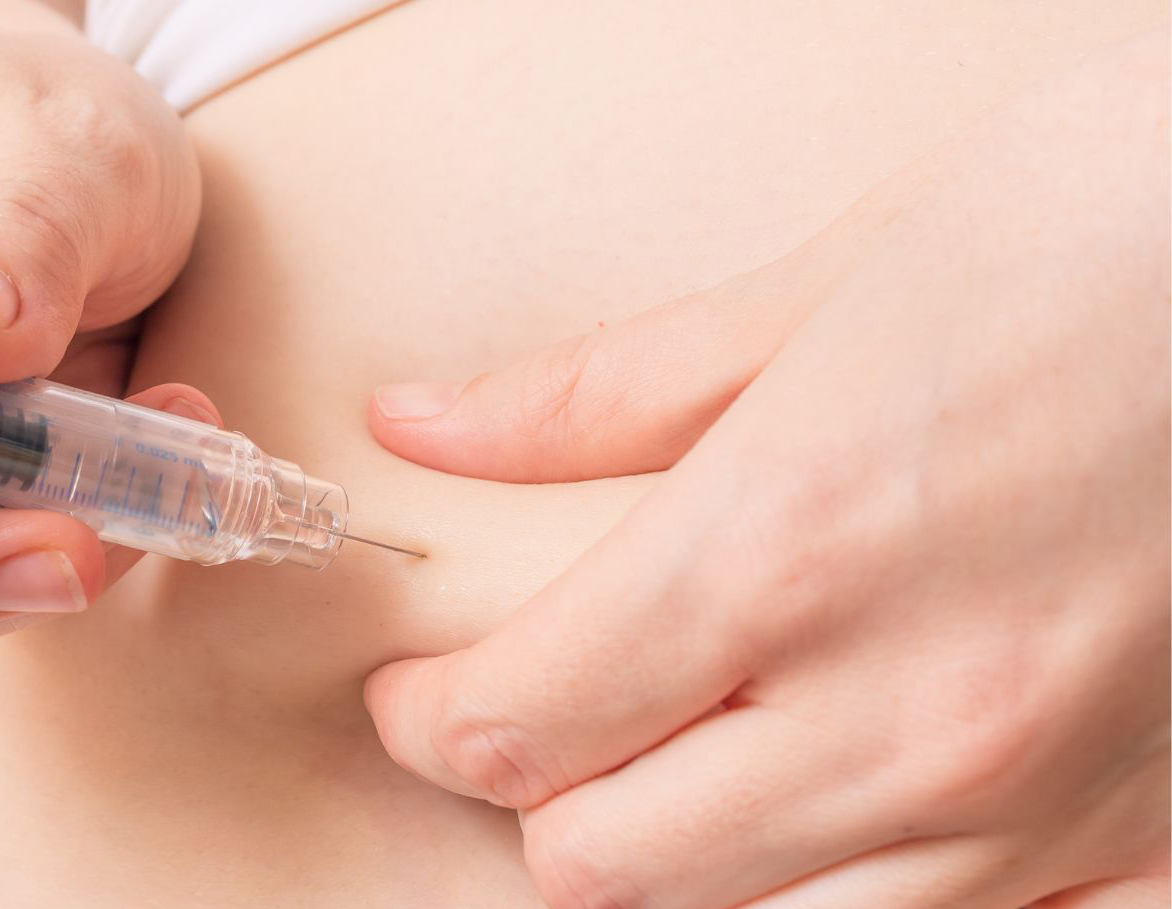
The aim of IVF is to stimulate the ovaries to develop several large follicles and then to mature the oocytes in the large follicles, so that the oocytes have the capacity to be fertilized by sperms. Stimulation is by gonadotrophins, which are hormones that stimulate the follicles to grow by action on receptors on the follicle. The hormones used in IVF are follicle-stimulating-hormone (FSH) and human menopausal gonadotrophin (hMG), which usually are produced and secreted from the pituitary (small gland that is attached to the brain: situated behind the eyes). The normal role of these hormones is to stimulate one follicle of each menstrual cycle to final growth so that ovulation occurs. In IVF, much higher hormone doses are given (by subcutaneous injections) than what is normal in a menstrual cycle. The consequence is that more than one follicle (often 5-10 per ovary) can develop to large antral follicles with oocytes that can mature and be fertilized. Transvaginal ultrasound is used to monitor the growth of the follicles, with the first scan performed around day 7 of stimulation and then with subsequent scan(s) depending on the findings at the first scan. When several follicles are above 17mm another hormone (hCG = human chorion gonadotropin or GnRH = gonadotropin-releasing hormone) is injected to induce final maturation of the oocytes, before they are retrieved from the follicle around 36 h later. There are two different gonadotropin stimulation protocols in clinical IVF today, the long- and the short-protocol.
Long stimulation protocol (agonist protocol)
The long gonadotropin stimulation protocol is also called the agonist protocol since a GnRH agonist is used. This was the classical stimulation protocol in IVF for many years but is more seldom used today, because of the higher risk of ovarian hyperstimulation syndrome (OHSS; see section below). The protocol typically starts in the middle of the time between ovulation and menstruation, which in a typical 28-days cycle is one week before the first day of menstruation. The medication taken then is a GnRH agonist, which usually is administered as a nasal spray, 2 or 3 times per day. This has a “flare up” effect on the secretion of FSH during the first week and the woman may sense these. Menstruation will come, but usually some days later than expected. After the flare up, when the nasal spray of the GnRH agonist has been taken around 3 weeks the ovaries will be downregulated since the levels of FSH will remain low. This is because the pituitary has been desensitized so that the numbers of GnRH-receptors is very low and there cannot be any signal to cause FSH release. The ovaries will only contain small follicles and produce very little estrogens, when they are downregulated. At this stage, the nasal spray is reduced to the half and gonadotropin stimulation will start. It usually takes around 11-12 days of gonadotropin stimulation until it is time to trigger follicle and oocyte maturation by an ovulatory trigger, in this protocol hCG acting on the LH receptors. Oocyte retrieval is around 36 h after hCG injection, with typically hCG at around 21:00 and oocyte retrieval at 09:00 two days later.
Short stimulation protocol (antagonist protocol)
The short gonadotropin stimulation protocol is also called the antagonist protocol since a GnRH antagonist is used. This is a more modern protocol than the long protocol. Typically, gonadotropin stimulation, by FSH or/and hMG, will start on the second or third day of menstruation. If the patient does not have regular menstruations this will be induced by progestin tablets or in some cases after using contraceptive pills. From the fifth day of stimulation, also a GnRH antagonist will be given to suppress the patient’s secretion of FSH and luteinizing hormone (LH), which could have given premature ovulation or luteinization (when the follicles produce progesterone too early). The stimulation will take around 10 days and then follicle and oocyte maturation will be triggered by either hCG or GnRH agonist, to give endogenous release of an ovulatory LH peak. Oocyte retrieval is around 36 h after hCG/GnRH injection.
What is ICSI
ICSI stands for intracytoplasmic sperm injection. It was invented by Dr. Palermo in 1991, when he was working in Brussels. The technique means that a sperm is injected into an oocyte to facilitate fertilization, in cases with poor (low count, low mobility) sperm samples. The invention of ICSI meant that most cases of male-factor infertility could be treated. ICSI can be combined with aspiration of sperms from epididymis or the testis (PESA/TESA), when no sperms are found in the ejaculated fraction.
What is happening in the laboratory after oocyte retrieval?
The embryologist will identify the oocytes in the follicular aspirates, collected at the oocyte retrieval (oocyte pick up (OPU)) procedure. The same morning the partner has produced a sperm sample to be brought to the laboratory. In cases of donor sperms, a frozen sperm sample will be thawed. After short culture/washing treatments of oocyte and sperms they will be incubated together in vitro in small droplets within covered, small plastic dishes. In cases of poor sperm sample ICSI will be performed. The fertilization rate of oocytes will be checked the morning after and fertilized oocytes will be further incubated in vitro, usually for 5 days to reach the blastocyst stage. At this stage, the embryo contains several hundred of cells, with an inner cell-mass giving rise to the fetus and an outer cell-mass giving rise to the placenta. Generally, one blastocyst will be transferred at ET (see below) and the other high-quality embryos will be frozen for later use in frozen ET cycles.
Side-effects of IVF, including OHSS
The most serious side effect of IVF is severe ovarian hyperstimulation syndrome (OHSS), which occurs in around 1% of cycles. It is more common after ovulation trigger by hCG than by GnRH. The clinical symptoms are abdominal pain, abdominal swelling and in some cases shortness of breath. The changes in the body are that the ovaries as well as the linings of the abdomen (peritoneum) and thorax (pleura) start to leak fluid and typically ascites (free fluid in the abdomen) will be seen together with very large ovaries. The collection of fluid in the “third space” (abdomen and in some cases also thoracic cavity) as well as changes in the coagulation system of the blood lead to an increased risk of venous thrombosis. These blood cloths can come at unusual locations such as the vein of the arm or in veins in the brain. Treatment with anticoagulation and drainage of fluid in the abdomen is often needed, as well as iv fluids to correct fluid balance within the blood system.Minor side-effects of IVF are pain in the lower abdomen with vaginal bleeding or infections after puncture of the vaginal wall and ovaries at oocyte retrieval.
Live birth chance of IVF
The chance of live birth after IVF is dependent on the age of the woman. The birth rate is usually expressed as birth rate per ET (embryo transfer) but it may also be of interest.what proportion of women achieves delivery of baby after IVF treatment started within a time interval after the first IVF treatment. This period may include more than one IVF stimulation and several ETs and will of course also include the time of pregnancy. In the Swedish quality registry of IVF (Q-IVF) 70% of women up to the age of 30 years achieved a live birth within 18 months, 60% of women of age 35 years and 25% of women of age 40 years. The birth rate per ET for the first ET in Swedish women are 37% for women below 30 years of age, 32% for women 31-35 years of age, 25% for women 36-37 years of age, 17% for women 38-39 years of age, 13% for women 40-41 years of age, and 8% for women 41 years of age or older.
How is a pregnancy after IVF?
A pregnancy of IVF should be regarded as a normal pregnancy and can be monitored by a midwife, according to clinical routines.
What are the costs of IVF in Sweden?
In Sweden, women under the age of 40 may have the right to publicly funded IVF. Women above 40 years of age or if they want a second child in a relationship have to seek medical help at a private IVF center. The current cost for one IVF treatment, including one fresh ET, and freezing of surplus embryos is about 40,000 SEK.

Article by
Mats Brännström
MD, PhD, Professor – Senior Consultant in Obstetrics and Gynecology
Other Articles

Samantha's Story
I knew from the start that it was hard to conceive a child of our own with my partner. As a child he... Read article

Male factor infertility
The definition of male factor infertility is when the cause of infertility within a couple is becaus... Read article

Endometriosis
The European Society of Human Reproduction and Embryology (ESHRE) has recently released an updated g... Read article
.jpg?alt=media&token=912e3772-6724-4c20-a29e-201478dda308)
Intrauterine Insemination
Intrauterine insemination (IUI), also called artificial insemination (AI), is a type of fertility tr... Read article

Jessica Olers's Story
Sometimes it doesn't turn out as planned. Ever since I was little, I have dreamed of a big family wi... Read article

Jessica’s Story
I have been pregnant three times. Or actually while writing this story, I am pregnant. But I don't f... Read article

Klara’s Story
Our infertility journey started two years ago. The process has not at all been what we expected and ... Read article
.jpg?alt=media&token=fc32a2e6-a127-4170-b5fb-b9338770ed1a)
The effects of Vitamin D on fertility
Vitamin D is a vitamin synthesized in the skin through sun exposure (UVB radiation). Moreover, vitam... Read article
Veronica’s Story
To make babies. Nowadays that phrase has a completely different meaning.In february 2019 we decided ... Read article

Tova’s Story
This is #mybumpystory - an emotional rollercoaster with repeated miscarriages and hopefully soon a b... Read article